Canadian Health Awareness Society : Resources
| Others - Contents |
| Others - Detail |
Hypothyroidism and Hyperthyroidism
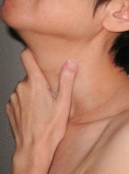
The thyroid is a butterfly-shaped gland in the front of the neck below the voice box. Its function is to produce thyroid hormone. There are two types of thyroid hormone T4 and T3. A gland in the brain called the pituitary gland controls the thyroid gland with a hormone call thyroid stimulation hormone or TSH. Thyroid hormone is responsible for metabolism, or the how the body use and store energy.
Cause of hypothyroidism: In 95% of cases, hypothyroidism is caused by disease in the thyroid gland itself and is called primary hypothyroidism. This is most commonly due to an autoimmune process. Hypothyroidism can also be due to certain medication. Surgery to remove parts of the thyroid, such as for thyroid tumors, also can result in hypothyroidism. Radioactive iodine, a treatment for hyperthyroidism/overactive thyroid, often leads to hypothyroidism as well. Much less commonly, disease in the pituitary gland results in secondary hypothyroidism.
Symptoms of hypothyroidism: Thyroid disorders are more common in women and in the elderly. Symptoms of hypothyroidism vary widely and effect many systems in the body. General symptoms of hypothyroidism include fatigue, low mood, weight gain, and intolerance of cold temperatures. An enlarged thyroid or goiter may be seen. Skin may become dry and thick. Hair and eyebrow thinning, and brittle nails may also be seen. Hypothyroidism can also slow down heart rate, raise blood pressure, and increase cholesterol. The digestive tract can be slowed as well, leading to constipation. Premenopausal women with hypothyroidism often have irregular periods, making it difficult to become pregnant. Hypothyroid women who become pregnant have an increased risk of miscarriage if untreated.
The severity of the above symptoms varies widely. Some people have little to no symptoms. However, hypothyroidism can be a life threatening condition in very rare cases. Myxedema coma is a rare life-threatening condition where thyroid function is very low, and typically exacerbated by exposure to infection, trauma or hypothermia.Diagnosis of hypothyroidism: Hypothyroidism is easily detected with a simple blood test for TSH, which is the best test to detect primary hypothyroidism. T4 can also be measured as well. TSH is tested in all newborn babies and women who are pregnant. It is also a common blood test done by family doctors with your annual physical check.
Treatment of hypothyroidism: Treatment of hypothyroidism is thyroid hormone replacement. This is given once per day in a pill form. It is best taken on an empty stomach 1 hour before eating or 2 hours after. Generic and brand name formulations are all effective. Symptoms generally improve within weeks of starting treatment.
The dose of thyroid hormone is dependent on the severity of hypothyroidism, weight, age and comorbid conditions. For example, elderly patients or patients with heart conditions generally receive a lower dose of thyroid hormone replacement since treatment makes the heart work a little harder. Pregnant women generally require higher dose as the baby needs thyroid hormone as well. Monitoring of thyroid blood test is done every 4-6 weeks until a stable dose is established. Blood tests can then be done every 6-12 months. Overdosing of thyroid hormone can be harmful, with increased risks of osteoporosis and irregular heart rhythm. Most people with hypothyroidism require life-long treatment.Hyperthyroidism is 5 times more common in women than in men. The overall prevalence is approximately 1.3%, and increases to ~5% in older women. It is also more common in smokers.
Causes of hyperthyroidism: There are primarily three causes of hyperthyroidism which we will outline here. Grave’s disease is the most common cause in younger patients. Grave’s disease is an autoimmune condition, where the immune system produces an antibody that stimulates the entire thyroid gland to make too much thyroid hormone. We do not know what cause the antibody to be produced. It is unrelated to diet or exercise.
Another cause of hyperthyroidism is hyperfunctioning thyroid nodules. This is a condition when the thyroid develops nodules or tumors that produce too much thyroid hormone. The rest of the thyroid gland functions other than the nodules function normally in this case. Hyperfunctioning nodules are more commonly seen in older patients. Although some thyroid nodules can be cancerous, hyperfunctioning nodules are never malignant.A third cause of hyperthyroidism is thyroiditis or inflammation of the thyroid. This is often seen after pregnancy or a viral infection. This can be thought of simply as they thyroid gland getting a “cold”. The inflammation leads to thyroid gland damage and hormone “leaking out” of the thyroid gland into the blood stream, and levels become too high. Note that this is different than the overproduction of thyroid hormone seen in Grave’s disease or hyperfunctioning nodules. After all the thyroid hormones leak out of the gland, there is often a period of hypothyroidism when the thyroid hormone levels are too low. However, the thyroid gland generally recovers to normal in several months in thyroiditis without treatment.
Symptoms of hyperthyroidism: As thyroid hormone plays a role in many organs, a wide range of symptoms can be seen in hyperthyroidism. The most common symptoms are weight loss, heat intolerance, excess sweating, increased appetite, insomnia, fatigue. In women, irregular periods, amenorrhea or infertility can be seen. In Grave’s disease, the eyes can be affected as well. Some patient’s with Grave’s develop change in the appearance of their eyes, where their eyes look “bulge out”, a condition called exopthalmous. The eyes can become watery, dry and irritated. In more severe cases, vision can be affected as well. Patient with Grave’s disease often have a diffusely enlarged thyroid gland due to the thyroid “working harder” then normal in making hormones. The thyroid gland can also be enlarged in patients with autonomous nodules due to the size of the nodules themselves. In thyroiditis, the thyroid gland is may be tender due to inflammation, and enlargement can sometimes be seen as well due to swelling from inflammation.
Diagnosis of hyperthyroidism: Hyperthyroidism is easily detected through blood test for levels of thyroid hormone. There are two types of thyroid hormones FT4 andFT3. One or both of these levels are elevated in hyperthyroidism. TSH or thyroid stimulating hormone is the signal from the pituitary gland in the brain that stimulates the thyroid gland. The TSH is low in hyperthyroidism as the brain does not need to stimulate the thyroid gland further as the thyroid hormone levels are already too high.
Additional tests are needed to determine the specific cause of hyperthyroidism. The antibody in Grave’s disease described above can be tested in blood test as well. If the antibody level is elevated, then Grave’s disease is very likely. A very useful imaging test is the radioactive iodine scan. This test involves the patient going to hospital to take a drink with radioactive iodine. The patient then can go home and then return to hospital a day later for a scan. Radioactive iodine accumulates in the thyroid gland and shows which part of the thyroid is overactive. In Grave’s disease, the entire thyroid gland is overactive. Whereas with hyperfunctioning nodules, only the nodules are overactive. In thyroiditis, the thyroid gland is actually not overactive at all as explained above, and this will be seen on the scan as well. Note that patients who are pregnant or breastfeeding cannot have radioactive iodine scan done.Treatment of hyperthyroidism: Once the exact cause of hyperthyroidism is determined, treatment can proceed. Patients are usually referred to an endocrinologist, or specialist in hormones for treatment. There are generally 3 options of treatment.
The first is taking a medication called Tapazole or PTU that slows down the thyroid gland. The dose of this medication needs to be adjusted regularly to ensure the thyroid hormone levels are not too high or too low. In Grave’s disease, a 12-18 month course of treatment with medication can lead to remission in ~30% of cases when the drug is stopped. In hyperfunctioning nodules, hyperthyroidism usually recurs when the medication is stopped.A second treatment option for Grave’s or hyperfunctioning nodule is called radioactive iodine ablation. This uses a stronger type of radioactive iodine than for the radioactive iodine scan. Patient who undergoes radioactive iodine ablation goes to the hospital to receive a stronger radioactive iodine drink. Precautions to avoid close contact with family members for a certain number of days will be discussed by the nuclear medicine physician. The stronger radioactive iodine will go to the thyroid and destroy the overactive parts of the thyroid gland. In Grave’s disease, radioactive iodine ablation leads to hypothyroidism in >90% of cases. Treatment with thyroid hormone will be required life long then. For autonomous nodules, patients are usually cured with radioactive iodine ablation. This is because the radioactive iodine destroys the activity of the hyperfunctioning nodules only and spares the rest of the thyroid gland. The rest of the thyroid gland can then function normally.
Removal of the thyroid gland with surgery is a much less commonly used option. This may be required if patient is allergic to anti-thyroid medication or have contraindication to receiving radioactive iodine ablation. Patients and their specialist will determine which of the above 3 options is best.